Why we created ThyroidScar Rx
Dr. Temmermand created ThyroidScar Rx out of necessity. During his 6 years of training in facial plastic surgery he struggled to find quality products that actually helped people reduce their scar appearance. Following the science of proven creams, lotions and tapes he found a list of ingredients and products that were proven to improve scars. But this still left him with issues. The available products only contained one or two useful elements and often a hodgepodge list was being recommended. Patients were sent scouring around to find these items and mixing them at home.
After performing hundreds and hundreds of thyroid and parathyroid surgeries, Dr. Temmermand got fed up giving this list of items for people to track down. He worked for over 1 year with a woman-owned, American cosmetics manufacturer to develop a novel scar cream that contained only scientifically proven ingredients into a balanced, gentle formula that would actually help people heal better. No gimmicks. No scams. Just science backed products to help his patients.
Read below about wound healing and the science behind this revolutionary formula. You'll also find useful blog posts, independent scientific information on the key ingredients in ThyroidScar Rx, and helpful FAQs regarding thyroid and parathyroid surgery.
Remember, you only get one chance to scar well. Don't miss your chance to have an excellent cosmetic outcome using scientifically proven products!
Blog posts
Post surgery care: what's important and what's not
Read more
Using the best closure techniques
Read more
How to place an incision for the best cosmetic result
Read more
How does a scar form?
Read more
Excellent nutritional status BEFORE surgery leads to BETTER healing
Read more
What makes for a good scar?
Read more
Scientific Research on Skin Healing & Scars
Zinc in wound healing
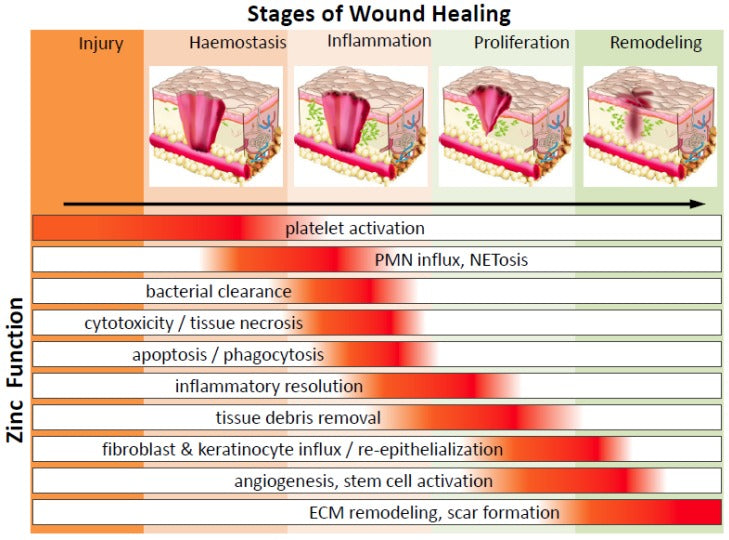
Zinc in Wound Healing Modulation
"Zinc is a micronutrient that is essential to human health. Zinc plays a major role in regulating every phase of the wound healing process; ranging from membrane repair, oxidative stress, coagulation, inflammation and immune defence, tissue re-epithelialization, angiogenesis, to fibrosis/scar formation.."
__
Lin PH, Sermersheim M, Li H, Lee PHU, Steinberg SM, Ma J. Zinc in Wound Healing Modulation. Nutrients. 2017 Dec 24;10(1):16. doi: 10.3390/nu10010016. PMID: 29295546; PMCID: PMC5793244.
--
Improved scar appearance with combined use of silicone gel and vitamin C
Improved scar appearance with combined use of silicone gel and vitamin C
"Facial scars, even fine surgical scars, often can be conspicuous and uncomfortable. The authors used a topical silicone gel containing vitamin C on facial scars for the purpose of making the scar less distinct. The results of the study show that topical use of silicone gel containing vitamin C has the effect of improving the appearance of fine surgical scars in Asian facial skin."
--
Yun IS, Yoo HS, Kim YO, Rah DK. Improved scar appearance with combined use of silicone gel and vitamin C for Asian patients: a comparative case series. Aesthetic Plast Surg. 2013 Dec;37(6):1176-81. doi: 10.1007/s00266-013-0210-5. Epub 2013 Oct 3. PMID: 24091488.
--
The role of Vitamin C in tissue healing
A Systematic Review on the Role of Vitamin C in Tissue Healing
"Tissue repair and regeneration within the body are influenced by vitamin C. A critical role of vitamin C is the synthesis of connective tissue, particularly collagen. It also provides tensile strength to new collagen formed which would otherwise be unable to stretch without tearing. In addition, vitamin C is an important antioxidant which can remove and neutralize oxidants in the body. This is particularly important in the epidermis.
Along with its role in collagen synthesis, there is also evidence that vitamin C increases the proliferation of dermal fibroblasts, a function important for wound healing."
--
Bechara N, Flood VM, Gunton JE. A Systematic Review on the Role of Vitamin C in Tissue Healing. Antioxidants (Basel). 2022 Aug 19;11(8):1605. doi: 10.3390/antiox11081605. PMID: 36009324; PMCID: PMC9405326.
--
The use of silicone sheets for scar reduction
The Use of Silicone Adhesives for Scar Reduction
"Results from clinical trials, now brought together through numerous reviews have strongly suggested that SGS are an effective preventative and reduction therapy for excessive scarring."
Why?
"SGS's ability to provide improved occlusion and hydration to the wound bed has been cited as its key physical mode of action in numerous studies. The physiological impact of improved occlusion and hydration on a developing scar is to provide the newly formed, underdeveloped stratum corneum aid in retaining optimum water levels. If the stratum corneum is dehydrated, it will signal to the keratinocytes in the epidermal skin layer to produce cytokines, which in turn signal fibroblasts to produce excessive amounts of collagen to aid water retention of the stratum corneum. It is by this process that the undesirable attributes of a hypertrophic scar are developed, rather than that of normal skin. Whereas it was once considered that higher occlusion is better, newer studies have shown that too strong a moisture barrier can have a detrimental effect, SGS is known to simulate the homeostasis of the stratum corneum. SGS, unlike other dressings, provide a level of occlusion similar to normal skin, which is thought to explain why cytokine and fibroblast activity and collagen formation are significantly reduced in SGS-treated scars and stratum corneum hydration is normalized. It is worth noting that the gentle removal of SGS compared with alternative adhesive sheeting also minimizes skin stripping of the newly formed stratum corneum, further contributing to its treatment potential.
Another physical mode of action provided by SGS is transferring tension from the lateral edges of the wound bed to the silicone gel sheet. The gentle reduction in tension which can be provided by an adhesive SGS provides the ideal environment for normal scar development and can significantly reduce the rate of abnormal and keloid scarring. Other treatments have the potential to apply too much or misplaced tension reduction, resulting in a poorer performance.
SGS has also been found to inhibit the body's natural reaction to increase skin capillaries through hyperemia. This reduces the blood supply to the scar site and the exaggeration of the healing process, along with the intensity of the fully formed scar's appearance and physical properties. The mechanism by which SGS has this effect has not yet been eluded, but research has prompted the idea that a significant temperature increase of the scar site is involved with the alteration of localized blood flow.
A final proposed mechanism of action is that SGS generates a negatively charged static electric field through the creation of friction between itself and the skin. This static electricity is thought to aid the alignment of collagen cells, thus resulting in the involution of raised scars."
--
Bleasdale B, Finnegan S, Murray K, Kelly S, Percival SL. The Use of Silicone Adhesives for Scar Reduction. Adv Wound Care (New Rochelle). 2015 Jul 1;4(7):422-430. doi: 10.1089/wound.2015.0625. PMID: 26155385; PMCID: PMC4486716.
--
Efficacy of topical silicone gel in scar management
Efficacy of topical silicone gel in scar management: A systematic review and meta‐analysis of randomized controlled trials
"Silicone gel has been used in scar management since the 1980 seconds. Silicone‐based products were deemed as the first‐line, gold standard therapy for scar management and have shown efficacy in both prevention and treatment of pathological scars."
"Topical silicone gel was significantly more effective in post‐operative scar prevention than placebos or no treatment when evaluated at 6 or more months after surgery, especially for height, pigmentation, and pliability relief."
"We recommend that at least 2‐month application of topical silicone gel is needed"
--
Wang F, Li X, Wang X, Jiang X. Efficacy of topical silicone gel in scar management: A systematic review and meta-analysis of randomised controlled trials. Int Wound J. 2020 Jun;17(3):765-773. doi: 10.1111/iwj.13337. Epub 2020 Mar 2. PMID: 32119763; PMCID: PMC7949016.
--
See also:
Puri N, Talwar A. The efficacy of silicone gel for the treatment of hypertrophic scars and keloids. J Cutan Aesthet Surg. 2009 Jul;2(2):104-6. doi: 10.4103/0974-2077.58527. PMID: 20808600; PMCID: PMC2918339.
--
Antioxidants in wound healing: Green tea extract, Allantoin, Aloe Vera, Vitamin E
A comprehensive evidence-based review on the role of topicals and dressings in the management of skin scarring:
"[Green tea extract] has a positive effect on wound healing"
"A study on Aloe Vera had found that average healing time and the re-epithelialization rate appeared to be reduced"
"The large prospective randomized single-blinded study by Zampieri (n = 428) assessed vitamin E both pre- and post-surgery in children. Utilizing the Vancouver Scar Scale, they summarized that treated wounds were of better appearance with less problematic scarring than the placebo group after 6 months."
--
Sidgwick GP, McGeorge D, Bayat A. A comprehensive evidence-based review on the role of topicals and dressings in the management of skin scarring. Arch Dermatol Res. 2015 Aug;307(6):461-77. doi: 10.1007/s00403-015-1572-0. Epub 2015 Jun 5. PMID: 26044054; PMCID: PMC4506744.
--
The evidence for natural therapeutics as potential anti-scarring agents in burn-related scarring:
"Moisturizing, anti-inflammatory, and immune-modulatory properties of the allantoin favor a dermo-protective and dermo-repairing action"
--
Mehta M., Branford O. A., Rolfe K. J. (2016).The evidence for natural therapeutics as potential anti-scarring agents in burn-related scarring.Burns Trauma.4, 15. 10.1186/s41038-016-0040-1
Sunscreen is essential in scar protection
Update on Postsurgical Scar Management:
"Newly formed scars less than 18 months old are highly susceptible to damage from ultraviolet radiation from the sun, causing hyperpigmentation and structural changes to the collagen matrix. This leads to a thickened and discolored scar. Minimizing sun exposure to the scar by covering with clothing or dressing is recommended. In addition, sunscreen with recommended SPF (sun protection factor) of 30 for 12 to 18 months postoperative is essential in protection against damaging ultraviolet radiation and must be worn at all times when the patient is in sunlight. Along with its main benefit of decreasing the risk of developing skin malignancy, sunscreen works to reduce scar hyperpigmentation by preventing melanogenesis, which occurs after ultraviolet light stimulation."
--
Commander SJ, Chamata E, Cox J, Dickey RM, Lee EI. Update on Postsurgical Scar Management. Semin Plast Surg. 2016 Aug;30(3):122-8. doi: 10.1055/s-0036-1584824. PMID: 27478420; PMCID: PMC4961501.
--
Hyaluronic Acid in scar healing
"It indicates that the combination of [silicone] and sodium hyaluronate resulting an improvement in anti-scar activity compared to the marketed product containing [silicone] alone."
--
AlamMS,AnsariA,AhsanI, et al.Topical gel containing Polysiloxanes and hyaluronic acid for skin scar: Formulation design, characterization, and In vivo activity.J Cosmet Dermatol.2023;22:1220-1232. doi:10.1111/jocd.15574
--
Parathyroid Surgery FAQs
Why have parathyroid surgery?
The most common reasons for people to have parathyroid surgery are for primary hyperparathyroidism (including adenomas, four gland hyperplasia, normocalcemic hyperparathyroidism, normohormonal hyperparathyroidism, and rarely parathyroid cancer), renal hyperparathyroidism and tertiary hyperparathyroidism.
Cancer of the parathyroid glands is very rare and is included under primary hyperparathyroidism
What is hyperparathyroidism?
Hyperparathyroidism is a condition where parathyroid hormone (PTH) is elevated.
There are 3 main causes of hyperparathyroidism: primary, secondary (includes renal) and tertiary. Primary hyperparathyroidism is the most common form and is characterized by an autonomously functioning gland or glands. Secondary hyperparathyroidism happens most commonly in patients with vitamin D deficiency and kidney failure. Lastly, tertiary hyperparathyroidism can be thought of as a renal hyperparathyroidism patient who then received a kidney transplant
What are the symptoms of primary hyperparathyroidism?
Symptoms of hyperparathyroidism can be broad and vague, often only being attributed to high calcium once the condition has been reversed. Some of the most common complaints are memory loss, fatigue, mental fog, depression, nausea, abdominal pain, constipation, diarrhea, bone pain, joint pain and muscle aches.
How is primary hyperparathyroidism diagnosed?
Diagnosis of primary hyperparathyroidism is almost entirely based off blood test. PTH levels compared to simultaneous blood calcium levels are most ciritcal. Vitamin D levels and kidney function are also useful. Sometimes, urine calcium levels can be helpful, too.
Imaging is NOT diagnostic for primary hyperparathyroidism and is NOT used to aide in the diagnosis.
Generally speaking, for primary hyperparathyroidism to be diagnosed one must have elevated calcium and a non-suppressed PTH level. Notice that PTH does not need to "elevated" above normal ranges. This is very confusing for non-specialists. Additionally, there are instances where calcium is normal and PTH remains elevated that we call normocalcemic hyperparathyroidism.
*Elevated calcium is age dependent. For example, a calcium over 10.0 in a 60 year old is often indicative of primary hyperparathyroidism while in a 25 year old would be normal. Just because the calcium is "normal" on the lab sheet does not mean it is okay.
What to expect before surgery?
The preoperative evaluation begins with reviewing lab test (blood work with calcium, PTH, Vitamin D and kidney function, and sometimes urine calcium levels in a 24 hour urine calcium test). After confirming that primary hyperparathyroidism is present a good surgeon will consider imaging such as a neck ultrasound and possibly additional imaging to include SPECT-CT, Sestamibi, 4D CT or Choline-PET scans.* The surgeon will also perform a painless evaluation of your vocal cords by using a small flexible camera inserted into the nose (Watch a video here).
Next, you should discuss all elements of the surgical process including risks, benefits and alternatives with specific regards to your personal medical, emotion and social needs. There is often some type of pre-operative testing needed for anesthesia ranging from simple blood work to EKG and "clearance" from any other doctors you might see (cardiology, pulmonology, primary doctor, etc)
*These tests are NOT diagnostic for primary hyperparathyroidism and the absence or presence of positive findings means zero in the indication for surgery.
How is parathyroidectomy performed?
Parathyroidectomy these days is performed via a minimally invasive approach as same day surgery.
After being put to sleep and a breathing tube is placed, the person is positioned lying flat on their back with the neck extended. The best cosmetic location for the incision is marked and the skin is sterilized. A baseline level of PTH is drawn as well.
A small incision (usually less than 1 inch) is made and the tissue below the skin is moved until the strap muscles of the neck are found. They are much like curtains that you have to part in order to see the thyroid gland. There you can move the thyroid out of the way to search for the parathyroid glands. The glands are inspected with direct visualization to determine if they are "good" or "bad" and removed if needed.
Once removed the PTH levels should be checked at set intervals (usually 5, 10 and 20 minutes after parathyroid gland removal). These are trended until the levels drop to an appropriate level. There is a common misconception that PTH levels must fall by 50% and into normal range to indicate cure. Do NOT be fooled by this. Statistically this is no better than removing a single gland and assuming you're done. Plus, this doesn't work when levels start in the normal range.
Some surgeons may use a radiotracer in the operating room that was injected prior to surgery. Rarely, methylene blue can be injected as well. Newer technology using autofluorescence is emerging but not yet ideal for true minimally invasive surgery.
After cure is achieved, the skin is closed cosmetically and the breathing tube is removed. The person is usually discharged home in a few hours.
What to expect after surgery?
After surgery most people can expect to have restrictions on physical activity for 5-7 days. Showering and wound care will vary depending on the surgeon and their closure technique. Similarly, returning to work will depend on the job duties and restrictions imposed. Driving usually resumes in 3-4 days.
Most people will have a light diet the night of surgery and resume all normal foods the following day. A light diet would be nothing too dense or fatty like fried chicken, for example. Soup, broth, shakes and pudding are on the lighter side.
There is usually some minor swelling at the surgical site. Major or significant swelling can indicate bleeding and should be reported to the surgeon immediately.
Pain is generally minimal after parathyroid surgery. Some people take a few opioid pain medications the day of surgery and acetaminophen the day after. Some take acetaminophen only. The throat tends to be sore from the breathing tube and is often more annoying that the incision.
A good idea of post-operative instructions can be found here.
What are the risks of parathyroid surgery?
Risks are generally related to the:
- Recurrent laryngeal nerves: there are two major nerves to your voice box and they bisect the parathyroid glands. They are infrequently injured during parathyroidectomy by skilled parathyroid surgeons. There is usually intraoperative monitoring of these nerves. Injury on one side can cause hoarseness, swallowing issues and sometimes shortness of breath. Injury to both sides usually leads to severe breathing problems and should be avoided.
- Parathyroid glands: these glands can be tricky to find and hide in places that are difficult to reach. Sometimes we have more or less than 4 parathyroid glands which can further complicate the surgery. While most of the time primary hyperparathyroidism will be caused by just 1 bad parathyroid gland (aka adenoma), it sometimes can be 2, 3 or all 4. If all 4 glands, and all are manipulated, it is possible to have HYPOparathyroidism after surgery. This requires one to take extra calcium pills to keep blood levels normal. This is rare.
- Pain: generally minimal after surgery. Throat pain from the breathing tube is often worse than the neck pain from the incision/surgery.
- Bleeding: exceedingly rare but could cause airway compromise if not addressed. Call your surgeon immediately if you have significant neck swelling after surgery. Bleeding during surgery is usually limited to a few drops.
- Infection: exceedingly rare but always a possibility.
- Anesthesia: general anesthesia is very safe these days, even for people with heart and lung conditions. This will have to be evaluated on an individual basis but for the most part is not really a concern.
- Cosmetic deformity (aka scarring): perhaps one of the worst parts of having parathyroidectomy. We always get scars on the skin when we cut it. This is inescapable. But we can manage it by hiding the scar in a crease, making incisions small, closing them using cosmetics techniques and treating the healing scar with creams, sunscreen and silicone tape.
Is parathyroid surgery painful?
Not much pain at all!
Generally this surgery is not very painful. Most people will take a few opioid pain medications the day of surgery and most people will take only acetaminophen the day following surgery. Many people have to be reminded to limit activity for 1 week since they feel so good in the days following surgery.
Is there an alternative to surgery for primary hyperparathyroidism?
Unfortunately, there is no substitute for removing the bad parathyroid gland(s) with a simple, outpatient surgery.
We can use a medication called Sensipar (cinacalcet) to lower the blood calcium levels which can help with symptoms and kidney stones, however the elevated PTH levels will remain and continue to damage the bones.
This medication is often only used as a temporizing measure since it only partially masks the disease. Additionally, it can be extremely expensive even with insurance.
How to find a parathyroid surgeon?
The best advice to finding an experienced parathyroid surgeon is to start with asking your endocrinologist who they trust (although they may be forced into referring internally within their health system despite that surgeon not being good at the procedure), Google, or Facebook groups dedicated to primary hyperparathyroidism. The Facebook groups keep lists of surgeons throughout the USA and even in other countries. There is also extensive support from the members of those groups.
A big university name does NOT equal a good parathyroid surgeon. Ask for how many they do each year and how many patients have persistent disease after surgery. They should perform a minimum of 50 parathyroid surgeries per year with cure rates >99%. Also, it is estimated that it takes around 200 parathyroid surgeries to gain sufficient experience to be successful at this procedure.
Many people will travel great distances to have a successful surgery on the first attempt.
The Thyroid & Parathyroid Surgery Center of New Jersey is one such place.
What happens if I don't treat parathyroid disease?
The main issues with not treating primary hyperparathyroidism is the continued damage to the bones leading to osteopenia and osteoporosis. Damage to the kidney will also occur in the form of kidney stones and kidney failure.
Other issues like psychological conditions such as anxiety & depression, memory loss, mental fog, abdominal pains, nausea, constipation, bone pain, joint pain and muscles aches may persist as well.
Imaging in primary hyperparathyroidism
This can be a very long discussion, but briefly said, imaging is an excellent adjunct to surgical exploration and can help expedite surgical times. It is NOT diagnostic for the condition and therefore "negative" imaging means nothing except all fours glands will need to be identified in the operating room. Conversely, "positive" imaging may still require all four gland to be identified during the surgery.
The most common types of imaging used are ultrasound, Sestamibi, SPECT-CT, 4D CT and Choline PET.
Ultrasound is painless, quick and safe. It should be performed by the surgeon. Normal parathyroid glands will not show up on ultrasound so anything found during the test will need to be evaluated intraoperatively. Ultrasound often allows for assessment of the thyroid gland as well since thyroid nodules are quiet common.
Sestamibi, and its more advanced cousin SPECT-CT, are tests done using an injected radiotracer. This tracer should absorb into glands or tissue with high mitochondrial density. It then typically "washes out" of those tissues as it is cleared from the body. Areas that retain the tracer can be indicative of overfunctional parathyroid tissue. The SPECT-CT version combines a standard Sestambibi scan with a CT scan to provide more detailed anatomy.
4D CT scan uses a different injected material called contrast. Then, a series of CT scans are performed to provide greater information regarding any areas of high tracer uptake. These can be very useful; however, finding an experienced radiologist to accurately read this scan is challenging.
A newer, and reportedly more sensitive test, is called a Choline PET scan. Finding one near you can be difficult and is typically very expensive (and sometimes not covered by insurance).
Could my high calcium represent cancer?
Most often, persistently elevated calcium levels in the blood indicate primary hyperparathyroidism. If the calcium is found to be elevated, a repeat blood test should be performed with a parathyroid hormone (PTH) drawn simultaneously.
If the PTH is suppressed, or appropriately low, relative to the calcium level you will need to find another cause. A rare condition to rule out are types of cancers that can produce a hormone similar to parathyroid hormone called parathyroid-related peptide (PTHrP). A simple blood test can be done for PTHrP.
99% of cases of primary hyperparathyroidism are caused by benign tumors called adenomas. Very rarely does this condition represent parathyroid cancer. Parathyroid carcinoma is classically characterized by very high calcium levels (13-18) and very high PTH (>300). More importantly, the diagnosis is confirmed in the operating room as parathyroid adenomas tend to be easy to remove while parathyroid carcinoma tends to be inseparable from the neighboring tissue, specifically the thyriod gland.
What should I do for my scar after surgery?
Scar healing is based on numerous factors, some of which you can control and others you cannot.
- Nutritional status - can be maximized by increasing protein intake, vitamin C and zinc prior to surgery.
- Health status - overall health impacts healing. Uncontrolled diabetes and smoking, for example, can lead to poor tissue healing and wound breakdown.
- Incision placement by surgeon - we scar 100% of the time the skin is injured. Good surgeons will use natural creases and neck shadows to hide scars for optimal cosmetic results.
- Closure techniques - using multilayered "cosmetics" closures, and excellent eversion and approximation of the skin edges allows for tension free healing.
- Post-operative care:
- Tension - tension across an incision puts stress on the healing tissue leading to wider, deep scars. Using silicone sheeting is one excellent and effective way to provide tension relief during scar maturation. Butterfly bandages also work well depending on the area and the degree of tension.
- Picking - picking at wounds including the scabs that form leads to additional scarring. The are best left alone in this regard. Clean crusting with 50/50 combination of hydrogen peroxide and clean water.
- Moisture - keeping wounds moist is fundamental to excellent healing. The skin is a moisture barrier and injuries such as incisions disrupt that function. Applying moisturizing agents to the scar 2-3 times per day helps tremendously. Look for ingredients such as hydrating hyaluronic acid and moisture barriers such as silicone.
- Local Nutrients - applying nutrients locally such as vitamin E and other antioxidants provide vital ingredients to help wound healing and fight off damaging free radicals. The skin is particularly sensitive to these damages during the healing phase.
- UV rays - these are damaging to even healthy, intact skin (regardless of your pigmentation). Using good SPF sunblock for the first 6-12 months is recommended, especially if direct sunlight is to be expected. With excessive exposure permanent hyperpigmentation can occur.
Thyroid Surgery FAQs
What are common reasons people have thyroid surgery?
The most common reasons people would have thyroid surgery are for goiters, nodules, Graves' disease and cancer.
How is Graves' disease managed?
Graves disease is an autoimmune condition where the thyroid becomes hyperfunctioning. The three main ways to manage Graves' disease are medications such as methimazole or propylthiouracil, radioactive iodine (RAI) or surgery to remove it.
What are "goiters?"
The term "goiter" is applied broadly to the thyroid gland when it contains multiple nodules or is enlarged. In the developed world, we don't know the exact cause of goiters but can be linked to autoimmune conditions such as Graves' disease or Hashimoto's thyroiditis, or can just happen. Iodine deficiency is a known cause but does not happen often in developed countries.
What is a thyroid nodule?
A thyroid "nodule" represents a lump inside the thyroid gland. These are extremely common and almost always benign (not cancer). They increase in prevalence as we get older. It is estimated that roughly 50% of the population over age 50 will have them.
We don't fully understand the reasons why they form but they can benign, solid, cystic, cancerous, pre-cancerous, or hyperfunctional.
The best way to "look" at thyroid nodules is with ultrasound. Ultrasound is a painless, radiation-free way to examine thyroid nodules. Depending on their characteristics (size, shape, density, etc) we can then decide if we should biopsy or just watch with repeat ultrasound.
Biopsy is done with ultrasound guidance and a very small needle. It is done in the office setting with no down time and usually results take 1-2 weeks. Thankfully, 95% of thyroid nodules are going to be benign.
What is a fine needle aspiration (FNA)?
Fine needle aspiration (FNA) is a simple, office based procedure that helps to figure out if a thyroid nodule is benign or cancerous.
A very fine needle is used to extract cells from the nodule and then examined by a pathologist. Usually a minimum of 2 needles are used per nodule. The process is generally not painful and has no down time.
The procedure is usually conducted by a patient lying down with the neck extended. It is then cleaned with alcohol and then either anesthetized with local anesthesia or the skin is anesthetized with topical spray. A small needle is inserted into the nodule using ultrasound guidance and cells are extracted. These are given to the pathologist to review.
What is thyroid cancer?
Thyroid cancer is a malignancy that develops in the thyroid gland. It occurs when thyroid cells undergo DNA mutations, causing them to grow and multiply uncontrollably, forming tumors. There are several types of thyroid cancer, including papillary (most common), follicular, medullary, and anaplastic. While the exact cause is often unknown, risk factors include radiation exposure, certain genetic conditions, and family history. Symptoms may include a lump in the neck, difficulty swallowing, voice changes, and neck pain. Diagnosis typically involves physical examination, imaging tests, and fine-needle aspiration biopsy. Treatment options depend on the cancer type and stage but often include surgery, radioactive iodine therapy, thyroid hormone therapy, and in some cases, targeted therapy or chemotherapy. Thyroid cancer generally has a good prognosis, especially when detected early. The overall survival rate is very high.
What to expect before thyroid surgery
Before having thyroid surgery one would need a thyroid ultrasound and often a biopsy of the thyroid gland. A CT scan can occasionally be useful, especially in the case of large goiters or potential spread of cancer.
A visit with a surgeon should include:
- Discussions regarding your case and specific needs (including medical history, surgical history and relevant personal and social history)
- Review of imaging
- Pathology if available
- Treatment options including risks, benefits and alternatives
- Discussion about the need or potential need for medication after surgery
- Possible repeat real-time neck ultrasound and flexible laryngoscopy [a painless evaluation of your vocal cords by using a small flexible camera inserted into the nose (Watch a video here)]
- Time for questions which should include asking for the number of cases that surgeon performs and what their rates of complications are such as injury to the recurrent laryngeal nerve and hypoparathyroidism
How is thyroid surgery performed?
Thyroid surgery is most commonly performed with an incision in the lower central neck and is often performed as a same day surgery. In almost all cases it is done under general anesthesia requiring a breathing tube. Standard of care is to use a breathing tube that allows for nerve monitoring to ensure the nerves to your vocal cords are protected. This means you would be completely asleep for the procedure.
Either half or the whole thyroid is removed leaving behind the parathyroid glands. All bleeding is controlled and then the skin is closed to ensure the best cosmetic outcome.
There are some potential options to avoid a lower neck incision though the availability is limited and the risk/benefit ratio is questionable in some. Remote access from behind the ear, armpit, breast and even through the mouth have been used. Transoral is the most popular alternative these days but still has a limited role
Is thyroid surgery painful?
Thyroid surgery is performed under general anesthesia so there is no pain during the actual procedure.
Afterwards, most people take opioid pain medications the day of surgery and possibly on the second day. On the second day a lot of people transition to acetaminophen only. Unfortunately the breathing tube needed for nerve monitoring during surgery causes a sore throat for 24-48 hours.
Interestingly, older people tend to need less pain medication than younger people after thyroid surgery.
Are there alternatives to thyroid surgery?
The only non-surgical alternative to thyroid surgery is a device called Radiofrequency Ablation (RFA). RFA is being used for non-cancerous nodules and is done in the office with some local anesthesia injected into the area. It is generally very well tolerated and seems to have had great success with shrinking thyroid nodules. Unfortunately, insurance coverage is not universal with out of pocket costs being $4000-5000 per treatment.
What are the risks with thyroid surgery?
The 3 top risks for thyroid surgery are the need for thyroid medication, hypoparathyroidism and nerve injury.
- Recurrent laryngeal nerves: there are two major nerves to your voice box and they run behind your thyroid gland (and sometimes through it). There is usually intraoperative monitoring of these nerves. Injury on one side can cause hoarseness, swallowing issues and sometimes shortness of breath. Injury to both sides usually leads to severe breathing problems and should be avoided.
- Parathyroid glands: we have 4 small organs in our neck called parathyroid glands that regulate our calcium levels. They are around the size of lentils. We need one of these glands to function so if all 4 got damaged it is possible to have HYPOparathyroidism after surgery. This requires taking extra calcium pills to keep blood levels normal. This is rare.
- Thyroid hormone pill: this a supplemental pill needed in 100% of cases with the entire thyroid removed and roughly 5-15% of people when half is removed. Occasionally, even after a partial thyroid removal one can need temporary supplementation of thyroid hormone while the remaining side is starting to function again.
The others risks are:
- Pain: generally minimal after surgery. Throat pain from the breathing tube is often worse than the neck pain from the incision/surgery.
- Bleeding: exceedingly rare but could cause airway compromise if not addressed. Call your surgeon immediately if you have significant neck swelling after surgery. Bleeding during surgery is usually limited to a few drops.
- Infection: exceedingly rare but always a possibility.
- Anesthesia: general anesthesia is very safe these days, even for people with heart and lung conditions. This will have to be evaluated on an individual basis but for the most part is not really a concern.
- Cosmetic deformity (aka scarring): perhaps one of the worst parts of having parathyroidectomy. We always get scars on the skin when we cut it. This is inescapable. But we can manage it by hiding the scar in a crease, making incisions small, closing them using cosmetics techniques and treating the healing scar with creams, sunscreen and silicone tape.
What is the recovery for thyroid surgery?
Generally most people should avoid heavy lifting, bending, jumping, stretching, and fighting for 1 week. Light activity the first week then no restrictions after that.
Most people won't feel safe to drive for 3-4 days due to limited neck mobility. You can talk and eat immediately, although it is advisable to have a light diet the night of surgery so as to avoid vomiting.
You can often return to work after 1 week. Some people will go light duty or remote login after day 3-4.
Showering depends on the closure technique used by the surgeon.
What are the long-term implications of thyroid surgery?
The major downside of having your thyroid removed is the need or potential need for replacement medication. If the whole thyroid gland is removed you will need thyroid hormone replacement. If half is removed the risk is generally around 5-15%.
Other long term implications are only related to potential complications.
How do I find a thyroid surgeon?
The best advice to finding an experienced thyroid surgeon is to start with asking your endocrinologist who they trust (although they may be forced into referring internally within their health system despite that surgeon not being good at the procedure). Sometimes Google can be useful, too.
A big university name does NOT equal a good thyroid surgeon. Many times they have trainees (aka residents) who perform the surgery for them. There are universities where the surgeon has two surgeries ongoing at the same time with the residents conducting the operation as they bounce back and forth between the rooms.
They should perform a minimum of 50 thyroid surgeries per year and have complication rates of permanent nerve injury less than 1% and permanent hypoparathyroidism under 1% (although these numbers may be slightly higher if their surgical population is mostly high risk cancer patients).
Many people will travel great distances to have a successful, uncomplicated surgery.
The Thyroid & Parathyroid Surgery Center of New Jersey is one such place.
What questions should I ask my doctor about thyroid surgery?
The questions to ask your surgeon would be:
- How many thyroids do you perform per year?
- For cancer or benign disease? What is the ratio?
- If you have cancer, ask what their experience is with removing lymph nodes in the neck?
- What are your rates of complications regarding nerve injury?
- What are your rates of complications regarding hypoparathyroidism?
- Will the surgery be same day or require a hospitalization?
- Do you use drains after surgery?
- How is the wound closed?
- Do you perform the surgery alone or with a PA/First assist/resident?
- How large do you anticipate the incision to be?
